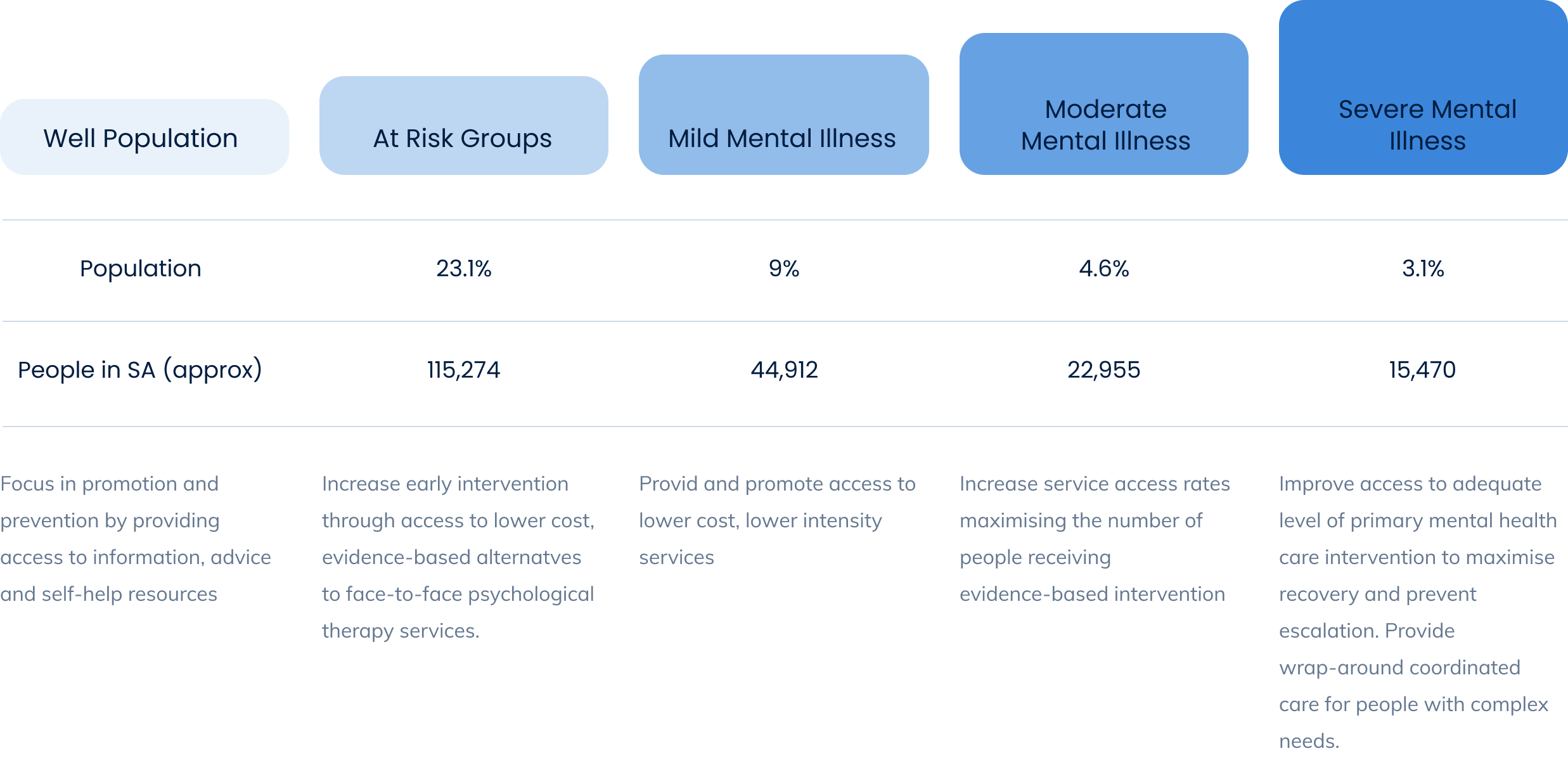
By introducing principles of stepped care across the State, we are able to focus on service delivery that matches the needs of individuals and has a particular emphasis on early intervention and self-care. That is, the person presenting to the mental health system is matched to the intervention level that most suits their current need.
They do not have to start at the lowest level of intervention in order to progress to the next step, rather they have their service level aligned to their requirements. Stepped care is defined as an evidence-based, staged system comprising a hierarchy of interventions, from the least to the most intensive, matched to the individual’s needs.
While there are multiple levels within a stepped care approach, they do not operate in silos or as one directional steps, but rather offer a spectrum of service interventions. In a stepped care approach, a person presenting to the mental health system is matched to the intervention level that most suits their current need.
An individual does not generally have to start at the lowest, least intensive level of intervention in order to progress to the next step. Rather, they enter the system and have their service level aligned to their requirements.